
Wildfires in the US are burning more land, burning longer, and reaching further than they did a generation ago. What used to be a regional, seasonal problem largely confined to parts of California and the Pacific Northwest now sends smoke across the entire country for weeks at a time. For people living with asthma or COPD, that shift isn't just an environmental headline. It's a direct respiratory threat that's getting harder to avoid, even if you never live near a fire.
Wildfires Are Getting Worse and So Is the Exposure
The scale has changed significantly.
According to the EPA, wildfire smoke now accounts for a growing share of poor air quality days across the US, affecting regions that historically had little exposure. Fire seasons that once ran a few months now stretch across much of the year in some states, and smoke from large fires regularly drifts thousands of miles reaching the Midwest, the South, and the East Coast.
For people with asthma or COPD, this means the window of risk is longer, less predictable, and no longer tied to where you live. You don't need to be near a fire to be affected by one.
Why Wildfire Smoke Hits Differently Than Regular Air Pollution
Most people assume wildfire smoke is basically bad air, unpleasant but not categorically different from smog or urban pollution. The science doesn't support that assumption.
The core concern is PM2.5, fine particles smaller than 2.5 micrometers that bypass the nose and throat entirely and penetrate deep into the lower airways and alveoli. What makes wildfire-specific PM2.5 particularly problematic is its chemical makeup.
Research published in Chest has found that wildfire smoke particles provoke stronger inflammatory responses in airway tissue than particles from vehicle exhaust or industrial emissions, due to higher concentrations of reactive organic compounds.
Wildfires also release gases that continue forming additional fine particles in the atmosphere after the visible smoke disperses, meaning actual pollution levels often exceed what AQI monitors show in real time.
Why Asthma and COPD Patients Are at Greater Risk
For most healthy adults, a smoky day means eye irritation and a cough that resolves once conditions improve. For the more than 25 million Americans living with asthma and 16 million with COPD (CDC), the situation is considerably more serious.
Both conditions share a key vulnerability: airways that are already inflamed, reactive, or structurally compromised at baseline. When wildfire smoke enters the picture, that pre-existing sensitivity tends to amplify the response.
Research has associated smoke exposure with acute asthma exacerbations, increased emergency department visits, and respiratory hospitalizations, with elevated risk observed particularly in older adults and those with pre-existing lung conditions.
For people with COPD, the concern extends beyond individual flare-ups. Repeated exposure to high PM2.5 concentrations has been associated with accelerated decline in lung function over time, according to findings in AJRCCM. Researchers are also examining whether long-term exposure to wildfires may play a role in COPD development in regions with recurring fire seasons.

The Problem With Indoor Air
Closing the windows doesn't fully solve it. Smoke particles are small enough to infiltrate homes through gaps around doors, windows, and HVAC systems, and indoor air quality during wildfire events can deteriorate significantly even when occupants believe they're protected. The EPA recommends HEPA air purifiers and high-rated HVAC filters (MERV-13 or higher) to reduce indoor PM2.5 during smoke events, but many homes don't have either.
This creates a real diagnostic gap. A patient who develops worsening symptoms while staying home might attribute it to stress, poor sleep, or just a difficult breathing day, never connecting it to smoke quietly accumulating inside. The trigger is invisible, the moment passes, and the pattern goes unrecognized. That misattribution matters: if you don't know smoke was driving your symptoms last time, you have no way to anticipate what's coming next.
When to See a Doctor
Seek care promptly if you notice your rescue inhaler becoming less effective, symptoms that continue to worsen despite staying indoors, chest tightness that persists overnight, or any significant change in breathing that doesn't improve when conditions clear. Smoke-related exacerbations can escalate faster than a typical flare. Don't wait to see if it resolves on its own.
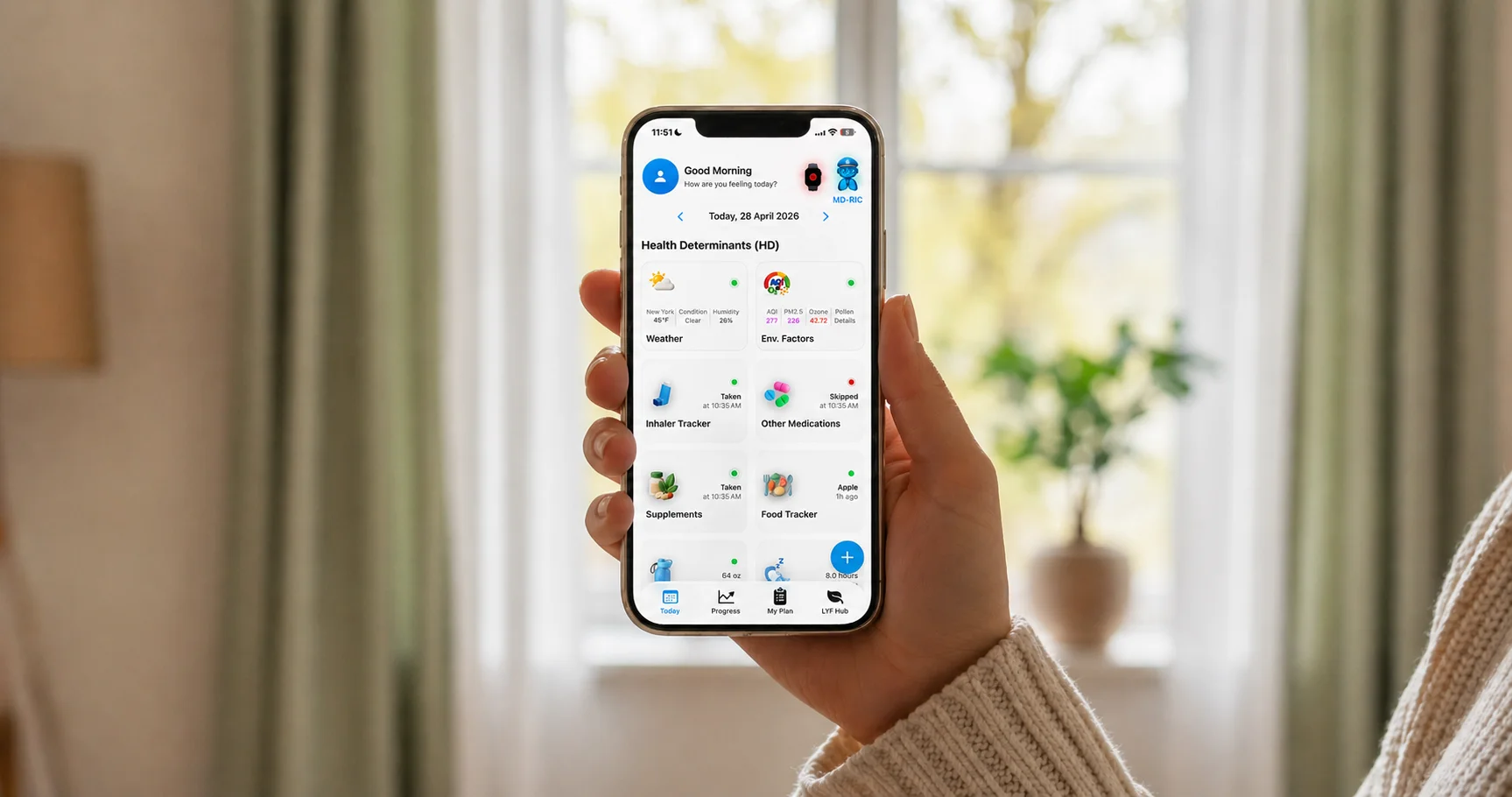
How Respire LYF Helps You Connect the Dots
This is exactly the kind of pattern that's hard to spot manually.
Your rescue inhaler use creeps up over three days. Sleep gets slightly worse. Your cough shifts. None of it feels alarming in isolation, but together, it points to something.
Respire LYF automatically tracks Weather & Environment as two of its 10 Health Determinants, pulling in local air-quality data alongside cough frequency, breathing score, sleep, inhaler use, and more. It analyzes these signals over time and surfaces correlations patients typically wouldn't connect on their own, including whether breathing tends to shift when PM2.5 rises, even subtly, even indoors.
Track What's Actually Affecting Your Breathing
Smoke season is longer now, and it reaches further. For people living with asthma or COPD, understanding how your airways tend to respond before the next event puts you in a better position when it does arrive. Tracking those patterns over time is how vague, frustrating weeks start to make sense.
Respire LYF is free to download on iPhone. It requires only a few minutes a day.
[Download Free on the App Store]
This article is for informational purposes only and does not constitute medical advice. Always consult your doctor or healthcare professional before making changes to your asthma or COPD management.