You took your controller medication last night, checked the forecast before bed, woke up to a clear sunny morning, and still couldn't take a full breath by 6 am. No smoke, no perfume, no obvious culprit. Just spring. If you've been asking yourself why my asthma is worse in spring, even when you're doing everything your doctor recommended, you're not missing something obvious. The answer is genuinely more complicated than "pollen is high," and once you understand what's actually happening, the bad days start to make a lot more sense.
You're Doing Everything Right, So Why Does Spring Still Wreck Your Breathing?
This is the part nobody talks about enough. Controller medications work by reducing baseline airway inflammation over time. They are not a force field. When spring arrives, it doesn't just add one new stressor; it layers several at once, and that combination can overwhelm even a well-managed respiratory system.
Your airways are already doing more work in spring than they do in January. The immune system is responding to allergens. The air quality is shifting daily. The weather is genuinely unstable. Your medication is still doing its job; it's just that the load placed on your lungs has increased significantly, and that gap is where the symptoms live.
This isn't a sign that your treatment plan is wrong. It's a sign that spring is a uniquely difficult season for people with asthma, and understanding why helps you respond smarter rather than just feeling blindsided.
Tree Pollen Is Only Part of the Problem
Tree pollen gets most of the blame for spring asthma flare-ups, and it deserves some of it. Oak, birch, cedar, and maple release enormous quantities of fine particles that, when inhaled, are associated with increased airway inflammation in people with asthma and allergies in spring.
Pollen counts can spike dramatically between 5 am and 10 am, which explains why so many people wake up symptomatic on mornings that look perfectly fine outside.
But here's what makes tree pollen especially tricky: it doesn't travel alone.
Pollen grains can absorb pollutants and carry them deeper into the airway than the pollen itself would reach.
On high-traffic days, pollen exposure tends to coincide with elevated particulate matter and ground-level ozone. Elevated ozone levels are associated with increased respiratory symptoms in people with asthma and COPD, so the two problems compound each other.
Mold spores also peak in spring as wet leaves decompose and soil warms. Grass pollen begins overlapping with tree pollen by late April in most of the US. By May, you may be responding to three or four airborne triggers simultaneously, and your body doesn't distinguish between them.
Why Spring Weather Itself Makes Things Unpredictable
This is the part that surprises most people. It's not just what's in the air, it's the air itself.
Spring weather is inherently unstable. Temperatures swing 30 degrees between morning and afternoon. Humidity spikes after rain and drops in the afternoon wind. Barometric pressure drops are associated with increased symptom reports in people with asthma, and spring produces more pressure fluctuations than almost any other season.
Cold, dry morning air followed by warm, humid afternoon air means your airways are adapting constantly. That repeated transition is irritating to already-sensitized tissue.
Then there's thunderstorm asthma, a phenomenon that sounds dramatic but is well-documented.
Thunderstorm events have been associated with spikes in asthma-related emergency visits in research studies.
The leading theory is that storm winds and electrical activity rupture pollen grains into much smaller fragments that penetrate deeper into the lungs than whole grains do. You can have a low official pollen count on a stormy day and still have a severe reaction, because the particles causing the problem are too small to be counted by standard monitoring.

The Real Reason Bad Days Feel Random: Environmental Stacking
Here's the concept that ties everything together: environmental stacking.
On any given spring morning, you might have moderate pollen, slightly elevated ozone, a humidity spike from overnight rain, and a pressure drop ahead of an afternoon front. None of those four things alone would necessarily cause a problem. But when they arrive together, the cumulative load on your airways crosses a threshold that a single trigger wouldn't reach.
This is why two days with identical pollen counts can feel completely different. The pollen count is one variable. The other variables, air quality index, humidity, temperature swing, and barometric trend, are changing independently, and they all interact.
It also explains why your medication seems to work fine in October but feels insufficient in April. The medication hasn't changed. The environmental load has.
Tracking these variables together, rather than checking pollen alone, is the only way to start seeing the actual pattern behind your worst days.
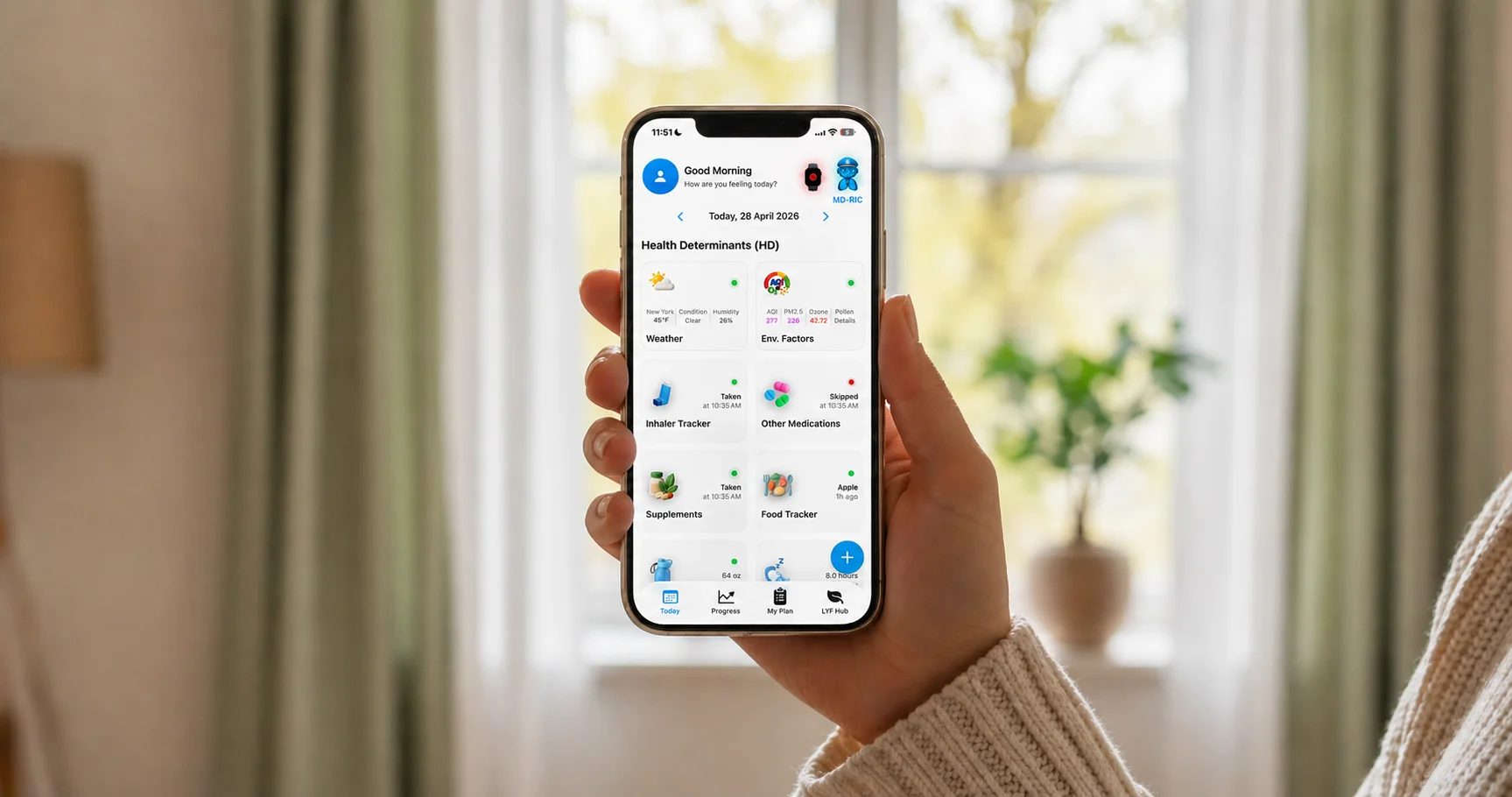
Respire LYF automatically logs the environmental factors (AQI, pollen) and weather (temperature, humidity) around you throughout the day, so you can look back at your worst breathing days and see exactly which combination preceded them. Over a few weeks, patterns that felt completely random start to become readable.
When to See a Doctor
A spring asthma flare-up that responds to your rescue inhaler and resolves within a few hours is worth monitoring, but a flare that doesn't respond is a different situation. Seek immediate medical attention if your rescue inhaler provides no relief after two treatments, if you're struggling to complete a full sentence, or if your lips or fingernails have any bluish tint. Chest tightness that wakes you repeatedly through the night, or symptoms that are significantly worse than your usual spring pattern, are also signs that your current treatment plan may need reassessment, not something to wait out. If you've needed your rescue inhaler more than twice in a single week, that's a conversation to have with your doctor before the season progresses further.
Track What's Actually Affecting Your Breathing
Understanding environmental stacking is useful. Having the actual data from your own days is what makes it actionable.
Most people with seasonal asthma are working from memory, trying to recall whether yesterday was worse, whether the windows were open, and whether it rained. Memory is unreliable, especially when you're symptomatic and fatigued. A log that captures your symptoms alongside the environmental conditions at the time gives you and your doctor something concrete to work with.
If you want to understand why my asthma is worse in spring on specific days rather than just in general, start tracking the full picture: breathing patterns, rescue inhaler use, sleep quality, and the environmental variables that were present. Over a season, that data tells a story that pollen counts alone never could. You can also review how your peak flow readings shift in relation to environmental conditions, and whether your nighttime symptoms cluster around specific weather patterns.
Spring doesn't have to feel like a mystery you're just enduring. The pattern is there; you just need the right data to see it.
[Download Free on the App Store →]
This article is for informational purposes only and does not constitute medical advice. Always consult your doctor or healthcare professional before making changes to your asthma or COPD management.
.webp)